Calm Skin [BONUS lesson ] The Stress–Pigmentation Connection: A Missing Piece in the Puzzle
For a long time, pigmentation has been taught as a largely topical issue.
We’re told it’s genetic.
That it’s bad luck.
That it’s caused by too much sun.
And that the solution is strong actives, peels, lasers, wide-brim sun hats, and patience.
I believed that too.
Dark patches on the skin, how could that possibly be influenced by diet, stress, or lifestyle?
But once you start understanding skin beyond the surface, something becomes very clear:
Everything is connected.
And pigmentation is not just a pigment problem.
It’s a communication problem.
~ and stress often sits right in the middle of that conversation.
Pigment cells don’t work in isolation
Melanocytes, the cells responsible for producing melanin, are often described as simple pigment-making cells.
In reality, they are highly sensitive, highly responsive, and deeply connected to the nervous system.
During early development, melanocytes and many nerve cells originate from the same starter tissue, known as the neural crest. You can think of them as distant cousins 👯♀️
Because of this shared origin, melanocytes can “listen” to many of the same chemical messengers used by the nervous system, including stress signals.
So when the body is under stress, whether physical, psychological, or emotional, melanocytes do not ignore it.
They respond.
How stress can directly increase pigmentation
When we experience stress, the brain switches on the body’s main stress response system, called the HPA axis.
HPA stands for hypothalamic–pituitary–adrenal axis. It is essentially a communication line between:
-
the brain, specifically the hypothalamus and pituitary gland
-
the adrenal glands, which sit on top of the kidneys
You can read more about the role of the HPA in skin barrier health and skin conditions here, here and here.
This system exists to help us cope with perceived threat. It once helped us run from danger. Today, it is just as easily activated by emails, deadlines, lack of sleep, or ongoing emotional stress.
When the HPA axis is activated, a cascade of chemical messengers is released.
Two of these are particularly relevant for pigmentation:
-
ACTH (adrenocorticotropic hormone)
-
α-MSH (alpha-melanocyte-stimulating hormone)
ACTH is released by the pituitary gland as part of the stress response. Its primary role is to signal the adrenal glands to produce cortisol, helping the body respond to stress. But it does not stop there.
α-MSH is closely related and, as its name suggests, directly stimulates melanocytes.
This is where pigmentation enters the picture.
How stress talks directly to pigment cells
Melanocytes have a specific receptor on their surface called MC1R (melanocortin-1 receptor).
You can think of MC1R as an antenna on the pigment cell.
When ACTH or α-MSH binds to this receptor, it sends a clear internal message:
Increase melanin production.
In other words, during periods of ongoing stress, the body can be chemically instructing pigment cells to stay active, even if sun exposure has not changed.
This helps explain why pigmentation can:
-
deepen during stressful periods
-
linger longer than expected
-
appear alongside inflammatory conditions such as acne or rosacea
-
Not improve for some clients even through they are following all of your advice
If UV exposure is also present, even low-grade everyday exposure, stress hormones can amplify the pigment signal. The result is darker or more persistent pigmentation than UV alone would typically cause.
Why this matters clinically
This pathway shows us that pigmentation is not only responding to light at the surface. It is also responding to internal stress signals. Influenced directly by your clients diet and lifestyle habits.
It helps explain why a client might be doing everything “right”. Avoiding the sun, wearing SPF daily, using appropriate skincare, yet progress still stalls.
If we only treat pigmentation topically, without addressing stress load, inflammation, and barrier resilience, we may be working against the biology rather than with it.
This pathway is especially relevant for clients experiencing:
-
acne with lingering pigmentation
-
inflammation alongside hyperpigmentation
-
pigmentation that feels stubborn or recurrent
It raises an important question:
🤔 Is stress driving both inflammation and pigment at the same time?
When stress and UV exposure coexist, even at low levels, stress can effectively add to the UV signal. At that point, the question shifts from:
Why won’t this pigmentation shift? 🤬
to:
What is continually telling these pigment cells to stay switched on? 🤨
A more helpful way to explain pigmentation
Rather than framing pigmentation as something that is “stuck” in the skin, I often explain it like this:
“Pigment cells respond to instructions. Those instructions come from light, inflammation, hormones, stress and skincare. When stress signals stay high, melanin production often stays high too.”
This perspective does two powerful things:
-
it guides more effective, long-term treatment strategies
-
it allows clients to understand their skin, rather than blame it
- empowers them with sustainaible strategies for long term skin health
No bad luck or dodgy genes.
No personal failure.
Just biology responding to the signals it is receiving.
And asking for something in its environment to change; that’s where you come in.
Why this matters for treatment outcomes
When pigmentation is treated purely from the surface, progress is often slow or short-lived.
But when we also support:
-
the skin barrier
-
nervous system regulation
-
inflammatory load
-
internal stress physiology
Working with pigmentation often becomes calmer, more predictable, and far more sustainable.
This is where true skin confidence is built, for both practitioner and client.
Key Takeaways:
I've summaried for you here, and also included a fascinating infographic if you, like me, are more of a visual learner. These are exactly the type of explanations you can expect inside SBS.
-
Pigmentation is not just a surface issue. It is influenced by internal communication pathways.
-
Stress activates the HPA axis, releasing hormones that can directly stimulate pigment cells.
-
Melanocytes are sensitive to stress signals due to their shared origin with nerve cells.
-
Stress can amplify the effects of UV exposure, leading to deeper or more persistent pigmentation.
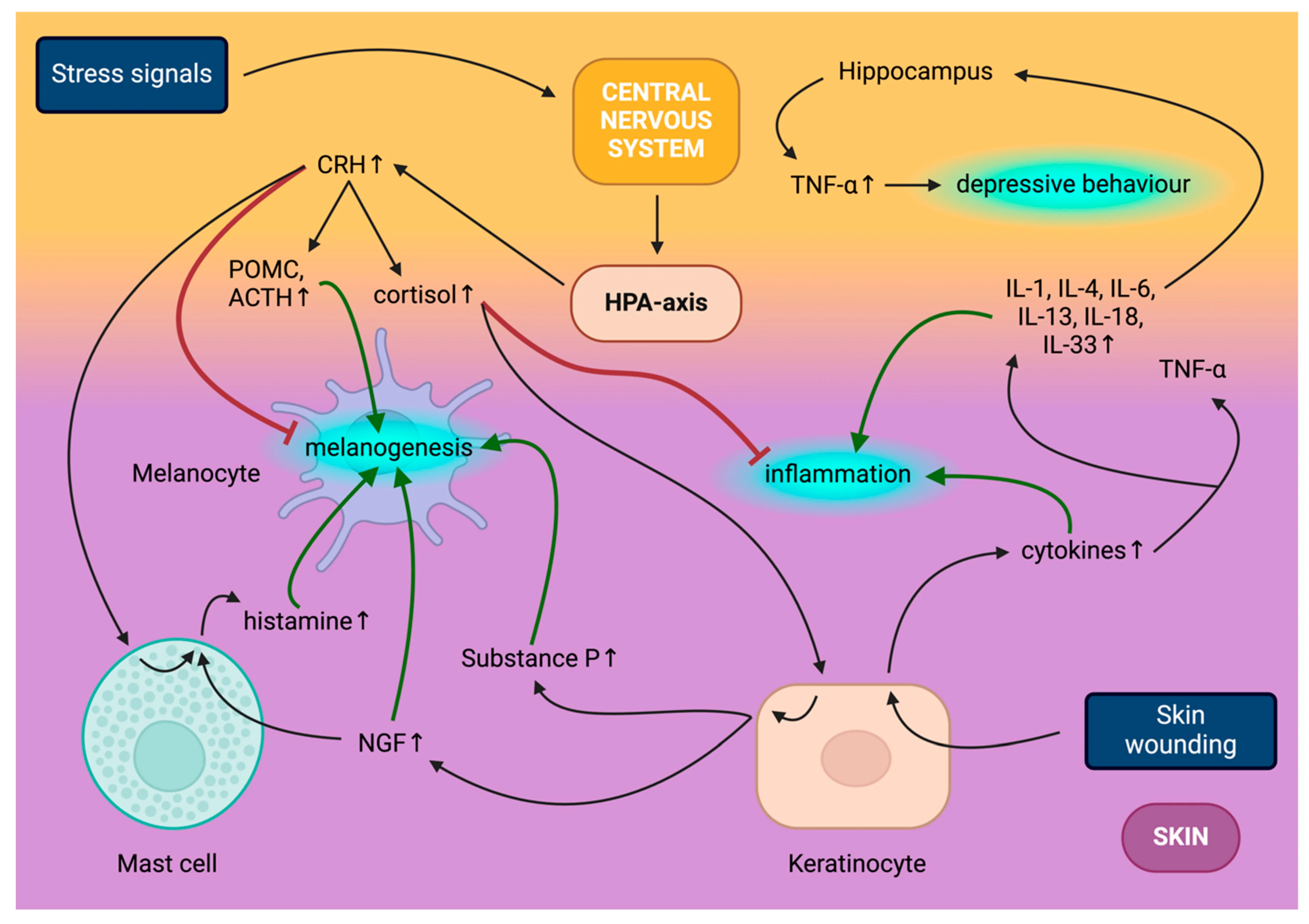
Ascsillán, A.A.; Kemény, L.V. The Skin–Brain Axis: From UV and Pigmentation to Behaviour Modulation. Int. J. Mol. Sci. 2024, 25, 6199. https://doi.org/10.3390/ijms25116199
Addressing stress, inflammation, and barrier health alongside topical care leads to more sustainable pigment outcomes.
Want to learn more about internal strategies to external skin problems? Join me for my free masterclass Beyond Skincare on Wednesday 21st January.
Chloe xx





Responses